Libri Bianchi & Pubblicazioni
Impegnati nella
ricerca scientifica
Libri Bianchi per alimentare il dibattito clinico, supportati da oltre cinquanta riferimenti scientifici: la prevenzione come approccio documentato.
Libri Bianchi · TBR
Tre Libri Bianchi,
un approccio documentato
Libro Bianco Vol.2 · 10/2025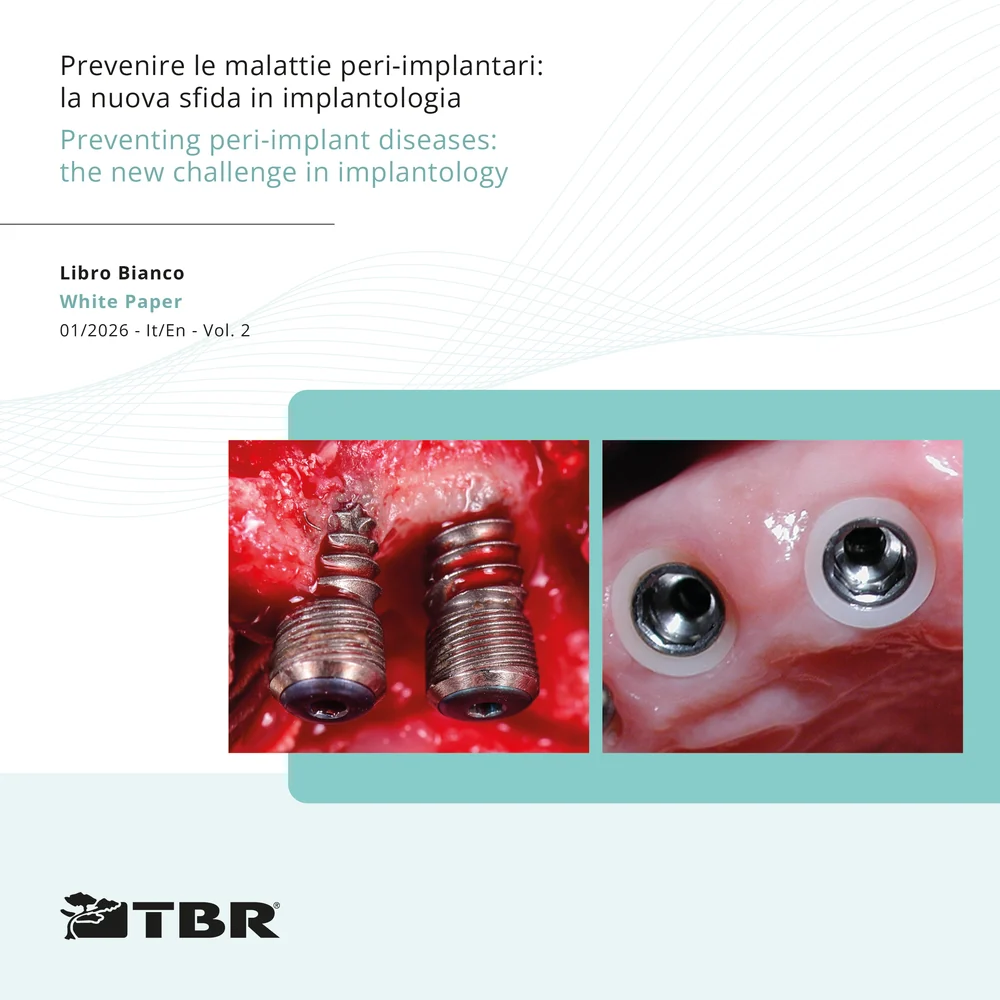


Prevenire le malattie peri-implantari: la nuova sfida in implantologia
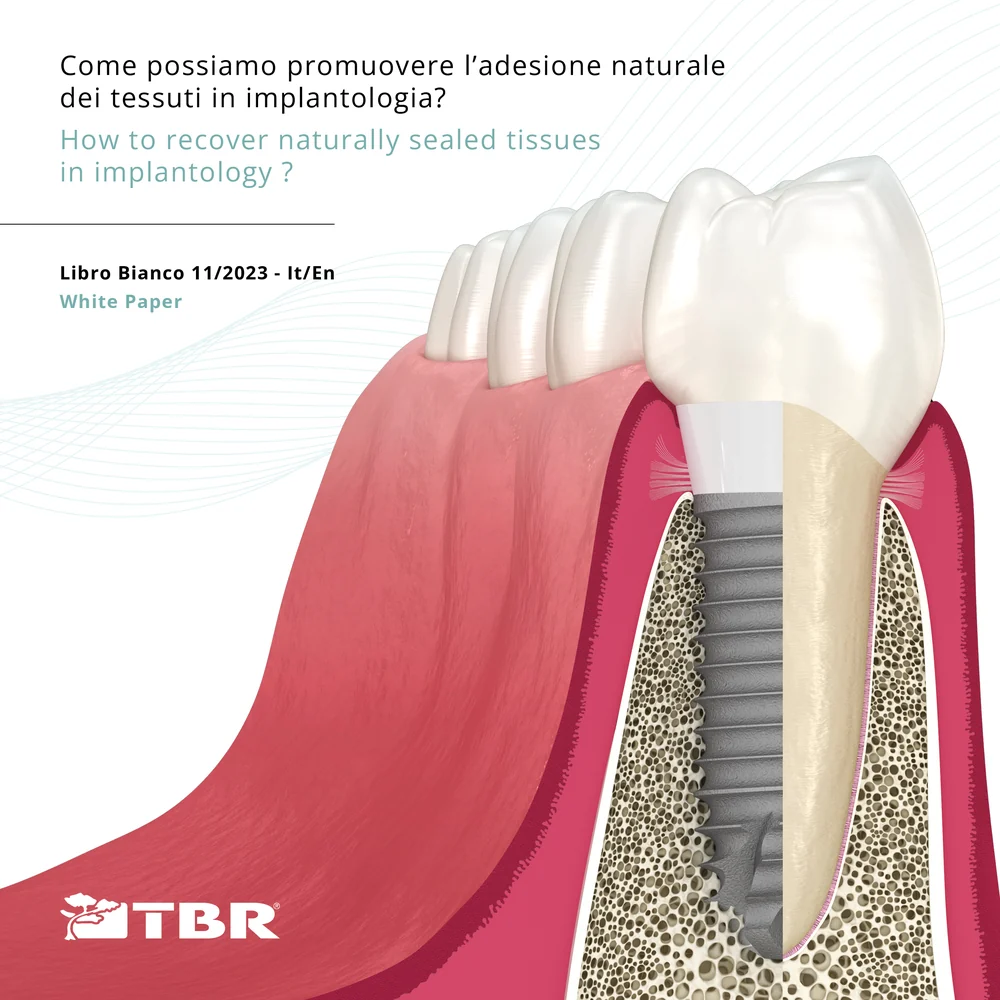
Scaricare il Libro BiancoLibro Bianco Vol.1 · 11/2023
Come possiamo promuovere l'adesione naturale dei tessuti in implantologia?
Scaricare il Libro BiancoLibro Bianco · 09/2024
Come rispondere oggi alla sfida dell'usura dei denti anteriori?
Scaricare il Libro BiancoPubblicazioni scientifiche
Oltre 50 riferimenti
peer-reviewed.
- S. Marconcini, E. Giammarinaro, N. Baldini, L. Canullo, and U. Covani. Clinical outcomes of post-extractive tissue-level implants with transmucosal zirconia collar: a prospective cohort study. Oral Maxillofac. Surg., vol. 30, no. 1, Mar. 2026. 10.1007/s10006-026-01551-7
- N. R. dos Reis et al. The prevalence of peri-implant mucositis and peri-implantitis based on the world workshop criteria: A systematic review and meta-analysis. J. Dent., vol. 160, p. 105914, Sept. 2025. 10.1016/j.jdent.2025.105914
- S. Al-Asaadi, N. Austin, P. J. Watson, D. J. Wood, A. Altaie, and F. P. Rodrigues. Titanium-Zirconia abutment-implant assemblies: Are they alternatives for single material implants? Dent. Mater., Jun. 2025. 10.1016/j.dental.2025.05.007
- Y.-H. Chou et al. Association between prosthesis contour and peri-implantitis in patients compliant with supportive periodontal therapy: A retrospective cohort study. J. Prosthodont. Res., Jan. 2024. 10.2186/jpr.jpr_d_23_00236
- J. Calatrava, I. Sanz-Sánchez, A. Molina, J. Bollain, C. Martín, and M. Sanz. Effect of one-time placement of the definitive abutment versus multiple healing abutment disconnections and reconnections during the prosthetic phase on radiographic and clinical outcomes: A 12-month randomized clinical trial. Clin. Implant Dent. Relat. Res., vol. 26, no. 5, pp. 998–1011, Jul. 2024. 10.1111/cid.13361
- L. J. A. Heitz-Mayfield. Peri-implant mucositis and peri-implantitis: key features and differences. Br. Dent. J., vol. 236, no. 10, pp. 791–794, May 2024. 10.1038/s41415-024-7402-z
- T. M. A. Al-Faraj et al. Comparison of peri-implant soft tissue around zirconia and titanium abutments in the aesthetic zone: A narrative review. Cureus, Jul. 2024. 10.7759/cureus.657
- F. Baudot. La corrosion des implants dentaires: facteur de risque des péri-implantites. Les implants zircone, une alternative préventive. Dental Tribune France, Oct. 2024.
- T. Steinherr. Implant Materials in Focus: A Comprehensive Review of Zirconia vs. Titanium and Their Impact on Peri-Implant Health. JOMDR, vol. 5, no. 4, Oct. 2024. 10.52793/jomdr.2024.5(4)-79
- S. Kumar, A. Singha, J. Dhingra, G. Verma, S. D. Singh, and A. Kumar. Evaluation of zirconia and titanium abutments on peri-implant tissues: A comparative study. Bioinformation, vol. 20, no. 12, pp. 1809–1812, 2024. 10.6026/9732063002001809
- C. Herráez-Galindo, M. Rizo-Gorrita, S. Maza-Solano, M.-A. Serrera-Figallo, and D. Torres-Lagares. Una revisione su CAD/CAM sul policristallo di zirconio tetragonale stabilizzato con ittrio (Y-TZP) e sul polimetilmetacrilato (PMMA) e sul loro comportamento biologico. Polymers, vol. 14, no. 5, p. 906, 2022. 10.3390/polym14050906
- S. Marconcini, E. Giammarinaro, J. A. Correia, A. Maltagliati, F. Salvado, and U. Covani. Titanium-Zirconia Tissue-level Implants in Patients with Well-controlled and Poorly-controlled Type 2 Diabetes: A cohort study with chair-side assessment of oxidative stress. Oral Implantol., vol. 15, no. 1, 2022.
- C. Pierre, G. Bertrand, I. Pavy, C. Rey, O. Benhamou, C. Roques, and C. Combes. Fosfato di calcio drogato di rame elettrodepositato: rivestimenti antibatterici per impianti dentali. J. Funct. Biomater., vol. 14, no. 1, p. 20, Dec. 2022. 10.3390/jfb14010020
- S. Shahdad, D. Bosshardt, M. Patel, N. Razaghi, A. Patankar, and M. Roccuzzo. Prestazioni di benchmark delle superfici implantari anodizzate rispetto a quelle sabbiate in un modello animale di difetto acuto di tipo deiscenza. Clin. Oral Implants Res., vol. 33, no. 11, pp. 1135–1146, Nov. 2022. 10.1111/clr.13996
- N. Mattheos, M. Janda, A. Acharya, S. Pekarski, and C. Larsson. Impact of design elements of the implant supracrestal complex (ISC) on the risk of peri-implant mucositis and peri-implantitis: A critical review. Clin. Oral Implants Res., vol. 32, no. S21, pp. 181–202, Oct. 2021. 10.1111/clr.13823
- J. Hu, I. Atsuta, Y. Ayukawa, T. Zhou, I. Narimatsu, and K. Koyano. Effetto degli abutment implantari in titanio o zirconia sugli attacchi epiteliali dopo la pulizia a ultrasuoni. J. Oral Sci., vol. 62, no. 3, pp. 331–334, 2020. 10.2334/josnusd.19-0332
- Y. Yi, K. Koo, F. Schwarz, H. B. Amara, and S. Heo. Association of prosthetic features and peri-implantitis: A cross-sectional study. J. Clin. Periodontol., vol. 47, no. 3, pp. 392–403, Jan. 2020. 10.1111/jcpe.13251
- A. Davarpanah. Le matrici CAD-CAM di tipo PICN (Polymer-infiltrated Ceramic Network): revisione bibliografica della letteratura e delle applicazioni cliniche. Sciences du Vivant [q-bio], Université Paris Descartes, 2019.
- L. Lago, L. da Silva, I. Martinez-Silva, and B. Rilo. Valutazione radiografica della perdita di osso crestale in impianti a livello tissutale ripristinati con Platform Matching rispetto agli impianti a livello osseo ripristinati con Platform Switching: A Randomized, Controlled, Split-Mouth Trial with 3-year Follow-up. Int. J. Oral Maxillofac. Implants, vol. 34, no. 1, pp. 179–186, Jan. 2019. 10.11607/jomi.6954
- D.-J. Lee, J.-S. Ryu, M. Shimono, K.-W. Lee, J.-M. Lee, and H.-S. Jung. Modelli di guarigione differenziale della mucosa su impianti in zirconia e titanio. Front. Physiol., vol. 10, p. 796, 2019. 10.3389/fphys.2019.00796
- C. Pierre, G. Bertrand, C. Rey, O. Benhamou, and C. Combes. Rivestimenti di fosfato di calcio elaborati mediante processo di immersione su impianti dentali in titanio: preparazione della superficie, lavorazione e caratterizzazione fisico-chimica. Dent. Mater., vol. 35, no. 2, pp. 25–35, Feb. 2019. 10.1016/j.dental.2018.10.005
- S. Chu et al. Restorative Emergence Profile for Single-Tooth Implants in Healthy Periodontal Patients: Clinical Guidelines and Decision-Making Strategies. Int. J. Periodontics Restorative Dent., vol. 40, no. 1, pp. 19–29, Dec. 2019. 10.11607/prd.3697
- M. Sanz et al. European Association for Osseointegration Delphi study on the trends in Implant Dentistry in Europe for the year 2030. Clin. Oral Implants Res., vol. 30, no. 5, pp. 476–486, Apr. 2019. 10.1111/clr.13431
- A. Maltagliati, F. Angiero, S. Zaky, S. Blasi, and A. Ottonello. Riduzione della proliferazione batterica mediante collare di zirconio negli impianti dentali. Annu. Res. Rev. Biol., vol. 23, no. 1, pp. 1–8, Jan. 2018. 10.9734/ARRB/2018/38270
- T. T. Vianna et al. Valutazione dei tessuti marginali perimplantari intorno agli impianti a livello tissutale e a livello osseo in pazienti con una storia di parodontite cronica. J. Clin. Periodontol., vol. 45, no. 10, pp. 1255–1265, Oct. 2018. 10.1111/jcpe.12999
- G. Da Gama Ramos, D. L. Ciotti, S. R. W. Ferreira, M. R. W. F. Margarido, R. A. Dantas, and M. N. Guerreiro. The use of a hybrid pillar and its importance for aesthetic rehabilitation and tissue stability: a clinical report. Case Reports in Dentistry, vol. 2018, pp. 1–6, Jul. 2018. 10.1155/2018/6850720
- M. Katafuchi, B. F. Weinstein, B. G. Leroux, Y. Chen, and D. M. Daubert. Restoration contour is a risk indicator for peri-implantitis: A cross-sectional radiographic analysis. J. Clin. Periodontol., vol. 45, no. 2, pp. 225–232, Oct. 2017. 10.1111/jcpe.12829
- A. Molina, I. Sanz-Sánchez, C. Martín, J. Blanco, and M. Sanz. The effect of one-time abutment placement on interproximal bone levels and peri-implant soft tissues: a prospective randomized clinical trial. Clin. Oral Implants Res., vol. 28, no. 4, pp. 443–452, Mar. 2016. 10.1111/clr.12818
- M.-A. Fauroux, C. Anxionnat, C. Biens, M. Mechali, O. Romieu, and J.-H. Torres. Le fonti della connessione implantare: confronto tra diversi tipi di impianti con il metodo della diffusione oculare. Rev. Stomatol. Chir. Maxillo-Faciale Chir. Orale, vol. 115, no. 2, pp. 74–78, Apr. 2014. 10.1016/j.revsto.2013.09.003
- P. Schüpbach. Interfacce tra tessuti e ceramica. Advanced Ceramics for Dentistry, Elsevier, 2014, pp. 201–217. 10.1016/B978-0-12-394619-5.00010-9
- S. Suryavanshi and M. Verma. Valutazione comparativa della risposta dei tessuti molli e dell'estetica degli impianti in titanio con zirconio. Maulana Azad Institute of Dental Sciences, New Delhi, Clinical Report, 2014.
- H. Su, O. Gonzalez-Martin, A. Weisgold, and E. Lee. Considerations of implant abutment and crown contour: critical contour and subcritical contour. Int. J. Periodontics Restorative Dent., vol. 30, no. 4, pp. 335–343, Aug. 2010. PMID 20664835
- S. Tetè, F. Mastrangelo, A. Bianchi, V. Zizzari, and A. Scarano. Orientamento delle fibre di collagene attorno a protesi dentarie in titanio e zirconia lavorate: An Animal Study. Int. J. Oral Maxillofac. Implants, vol. 24, no. 1, pp. 52–58, 2009.
- A. E. Bianchi, M. Bosetti, G. Dellavia, M. T. Sberna, F. Sanfilippo, and M. Cannas. Follow-up in vitro e in vivo di impianti transmucosi in titanio con collare in zirconia. J. Appl. Biomater. Biomech., vol. 2, no. 3, pp. 143–150, 2004.
- L. Rimondini, L. Cerroni, A. Carrassi, and P. Torricelli. Colonizzazione batterica delle superfici ceramiche di zirconia: uno studio in vitro e in vivo. Int. J. Oral Maxillofac. Implants, vol. 17, no. 6, pp. 793–798, 2002.
- J. S. Hermann, D. Buser, R. K. Schenk, F. L. Higginbottom, and D. L. Cochran. Ampiezza biologica intorno agli impianti in titanio: una dimensione fisiologicamente formata e stabile nel tempo. Clin. Oral Implants Res., vol. 11, no. 1, pp. 1–11, Feb. 2000. 10.1034/j.1600-0501.2000.011001001.x



